Every week, patients walk into my clinic confused about one thing: “Doctor, mujhe Type 1 hai ya Type 2?” And honestly, that confusion is completely understandable. The names sound similar, but these are two very different conditions with different causes, different treatments, and very different long-term journeys.
Whether you have just been diagnosed, or a family member is living with diabetes, understanding this difference could genuinely change how you approach your health. In this guide, I will walk you through everything you need to know, from causes and symptoms to diagnosis and treatment, in plain, simple language.
What is Diabetes?
Diabetes is a chronic condition where the body cannot properly regulate blood sugar (glucose) levels. Glucose is the fuel your body runs on, and insulin (a hormone made by the pancreas) is what helps your cells absorb and use that fuel.
When this system breaks down, blood sugar stays dangerously high. Over time, this can silently damage your nerves, kidneys, eyes, heart, and blood vessels.
Dr. Verma says: In my 20+ years of practice, I have seen how uncontrolled blood sugar damages the body quietly, often without symptoms until it is too late. That is why early awareness and timely testing matter more than people realise.
Role of Insulin in Blood Sugar Control
Think of insulin as a gatekeeper. When you eat, your blood sugar rises. The pancreas releases insulin, which signals cells across your body to open up and absorb glucose for energy. In people with diabetes, this gatekeeper is either missing or not working properly, and blood sugar keeps rising with nowhere to go.
What is Type 1 Diabetes?
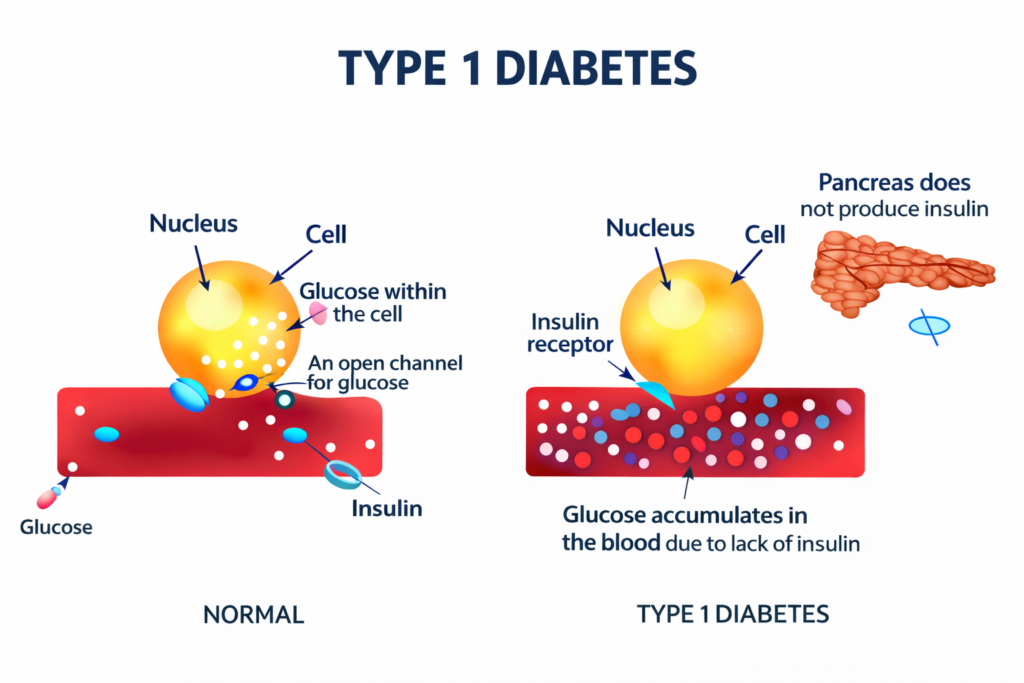
Type 1 diabetes is an autoimmune condition where the body’s own immune system mistakenly attacks and destroys the insulin-producing cells in the pancreas. The result: the body produces little to no insulin at all. People with Type 1 diabetes need insulin every single day to survive.
This was previously called juvenile diabetes, but it can develop at any age, not just in children or teenagers.
Causes of Type 1 Diabetes
- Autoimmune response that destroys pancreatic beta cells
- Genetic predisposition
- Possible environmental or viral triggers
- Family history of Type 1 diabetes
Symptoms of Type 1 Diabetes
- Extreme thirst and frequent urination
- Rapid, unexplained weight loss
- Blurred vision
- Fatigue and weakness
- Fruity-smelling breath (a sign of diabetic ketoacidosis)
Dr. Verma says: Type 1 symptoms often appear suddenly and can become serious within days. Parents, if your child is losing weight rapidly, urinating more than usual, and seems unusually tired, please do not delay. Get a blood sugar test done immediately.
Risk Factors for Type 1 Diabetes
- Family history of the condition
- Certain genetic markers
- History of specific viral infections
What is Type 2 Diabetes?
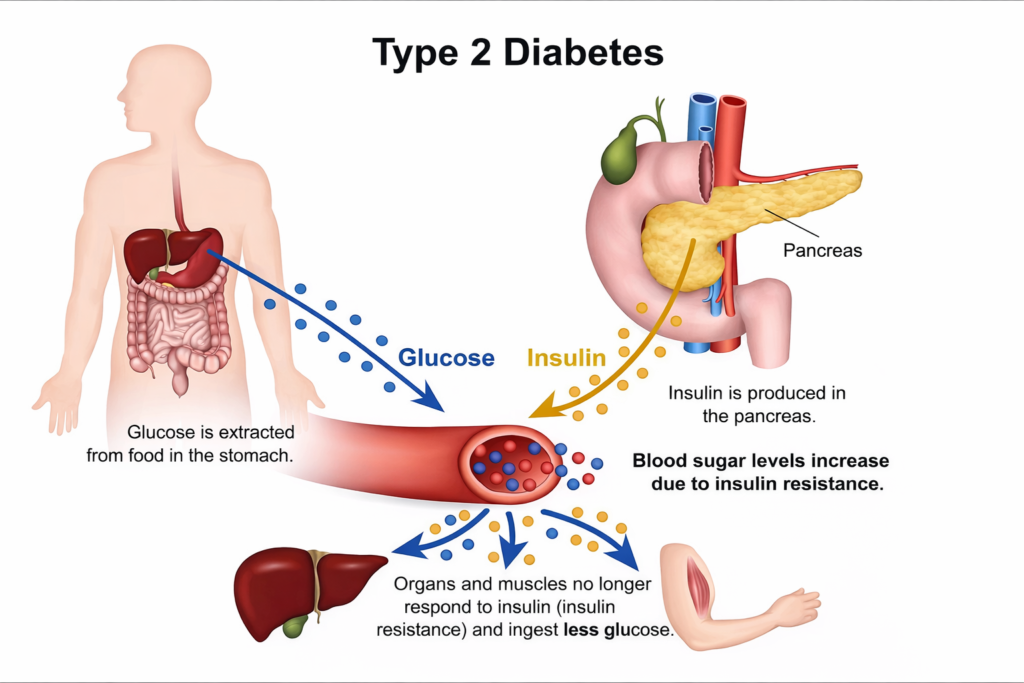
Type 2 diabetes is by far the most common form, accounting for over 90% of all diabetes cases. Here, the body either does not produce enough insulin, or the cells stop responding to it properly. This is called insulin resistance.
Unlike Type 1, Type 2 develops gradually and is strongly linked to lifestyle. With the right changes, many patients can manage it very effectively and sometimes even achieve remission.
Causes of Type 2 Diabetes
- Insulin resistance: cells stop responding to insulin effectively
- Excess body weight, especially around the abdomen
- Physical inactivity
- Unhealthy diet high in sugar and refined carbs
- Genetic factors and family history
Symptoms of Type 2 Diabetes
- Increased thirst and urination
- Slow-healing wounds or frequent infections
- Tingling or numbness in hands and feet
- Darkened skin in body folds (acanthosis nigricans)
- Fatigue and blurry vision
Dr. Verma says: The tricky thing about Type 2 diabetes is that many patients feel perfectly fine for years. By the time they notice symptoms, the blood sugar has already been high for a long time. This is why I always recommend proactive testing, especially if you are above 40 or have a family history.
Risk Factors for Type 2 Diabetes
- Age above 45 years
- Overweight or obesity
- Sedentary lifestyle
- Family history of Type 2 diabetes
- High blood pressure or cholesterol
Type 1 vs Type 2 Diabetes: Key Differences
Here is a quick side-by-side comparison to help you see the core differences clearly:
| Feature | Type 1 Diabetes | Type 2 Diabetes |
| Cause | Autoimmune | Insulin resistance |
| Onset | Sudden | Gradual |
| Age | Usually young | Usually adults |
| Insulin | Required | Sometimes |
| Prevention | No | Often yes |
Symptoms of Type 1 vs Type 2 Diabetes
While both types share some symptoms, how and when they appear is quite different:
Type 1 Diabetes:
- Sudden onset, rapid weight loss, risk of diabetic ketoacidosis (DKA)
- Intense thirst and very frequent urination
Type 2 Diabetes:
- Gradual development over months or years, often with no obvious symptoms early on
- Slow-healing sores, tingling in extremities, darkened skin patches
Diagnosis of Type 1 vs Type 2 Diabetes
Accurate diagnosis is the foundation of good treatment. These are the three tests most commonly used:
A1C Test
This test shows your average blood sugar over the past 2 to 3 months. A result of 6.5% or above on two separate occasions confirms diabetes. It is one of the most reliable tools we use.
Fasting Blood Sugar Test
Blood glucose is measured after an overnight fast of at least 8 hours. A level of 126 mg/dL or higher on two occasions confirms a diabetes diagnosis.
Oral Glucose Tolerance Test
After fasting, you drink a sugary solution and your blood sugar is tested 2 hours later. A result of 200 mg/dL or above indicates diabetes. This test is particularly useful for detecting gestational diabetes.
Treatment for Type 1 Diabetes
Since the pancreas cannot produce insulin in Type 1, treatment is built around replacing that insulin safely and effectively:
Insulin Therapy:
Insulin is non-negotiable for Type 1. It is delivered through multiple daily injections or an insulin pump, using different types such as rapid-acting and long-acting insulin depending on individual needs.
Blood Sugar Monitoring:
Regular monitoring using a glucometer or a Continuous Glucose Monitor (CGM) helps patients keep their levels in a safe range and make timely adjustments to insulin doses.
Diet and Exercise:
Carbohydrate counting and consistent physical activity help stabilize blood sugar. Exercise needs to be planned carefully, as it can cause blood sugar fluctuations in Type 1.
Treatment for Type 2 Diabetes
Type 2 treatment starts with lifestyle first, and steps up from there based on how the body responds:
Lifestyle Changes:
A balanced diet and at least 150 minutes of moderate exercise per week can significantly improve insulin sensitivity. For many patients, this alone makes a meaningful difference.
Medications:
Oral medications like Metformin are commonly prescribed as a first step. Newer drug classes such as SGLT2 inhibitors and GLP-1 receptor agonists have also shown benefits for heart and kidney health. Learn more about treatment options at Dr. Dileep Verma’s diabetes clinic.
Weight Management and Insulin:
Losing even 5 to 10% of body weight can dramatically improve blood sugar control. In advanced cases where the pancreas is struggling, insulin therapy may also be added.
Dr. Verma says: I always tell my Type 2 patients: medication is a support tool, not a replacement for lifestyle. The patients who do best are the ones who take ownership of their diet and movement. Tablets work best when paired with healthy habits.
Can Type 2 Diabetes Turn Into Type 1?
No. This is one of the most common myths I hear in my clinic, and I want to set it straight. Type 2 diabetes cannot convert into Type 1. They are entirely separate conditions with different root causes.
Some people with Type 2 eventually need insulin, and this is often misunderstood as ‘becoming Type 1.’ In reality, they still have Type 2; their pancreas just needs extra support. There is also a lesser-known condition called LADA (Latent Autoimmune Diabetes in Adults) that behaves like Type 2 at first but has an autoimmune origin, similar to Type 1. It is worth ruling out with the right tests.
Which is More Dangerous: Type 1 or Type 2?
Both are serious. Neither is ‘mild.’ Type 1 carries the risk of diabetic ketoacidosis (DKA), a medical emergency that can develop rapidly if insulin is missed. Type 2, if left poorly managed, can silently damage the heart, kidneys, nerves, and eyes over years.
The honest answer is: the danger in both lies in neglect. Managed well, people with either type can live full, healthy lives. The key is awareness, regular monitoring, and staying consistent with your treatment plan.
Prevention Tips for Type 2 Diabetes
Type 2 diabetes is largely preventable. Here is what I guide my at-risk patients to focus on:
Healthy Diet:
- Cut down on sugar, refined carbs, and ultra-processed foods
- Add more vegetables, fiber-rich foods, legumes, and healthy fats to your plate
Regular Exercise:
- Aim for at least 30 minutes of moderate activity, 5 days a week
- Even a 20-minute walk after meals helps lower post-meal blood sugar
Weight Control:
- Keep your BMI under 25 and pay attention to belly fat, which is a key driver of insulin resistance
Regular Screening:
If you are above 40, overweight, or have a family history of diabetes, get your fasting blood sugar and HbA1c tested every year. Catching pre-diabetes early gives you the best possible window to reverse the course. You can schedule a screening with Dr. Dileep Verma here.
Frequently Asked Questions
What is the main difference between Type 1 and Type 2 diabetes?
Type 1 is an autoimmune condition where the body produces no insulin at all. Type 2 is a metabolic condition where the body produces insulin but cannot use it effectively. Type 1 always requires insulin from the start; Type 2 can often be managed with lifestyle changes and oral medication.
Can Type 2 diabetes be reversed?
In many cases, yes. Significant weight loss, dietary changes, and regular exercise can bring blood sugar back to normal levels without medication, a state called remission. It does not mean the risk is gone permanently, but it is absolutely achievable with consistent effort and medical guidance.
Do Type 1 diabetics always need insulin?
Yes, always. Since the pancreas in Type 1 does not produce insulin, it must be supplied externally every day. There is currently no cure, though research into islet cell transplants and artificial pancreas technology is progressing.
Which diabetes is genetic?
Both types have a genetic component. Type 1 has a stronger autoimmune genetic link, while Type 2 is influenced by both genetics and lifestyle. Having a parent with Type 2 diabetes roughly doubles your risk, but the good news is that lifestyle choices can significantly reduce that risk.
Can children develop Type 2 diabetes?
Yes, and it is becoming increasingly common. Rising rates of childhood obesity mean that Type 2 diabetes is now being diagnosed in teenagers and even younger children. Healthy eating habits and daily physical activity from an early age are the most powerful protection.
Conclusion
Type 1 and Type 2 diabetes are fundamentally different conditions, but they share one common truth: early awareness and consistent care make all the difference. Whether it is an autoimmune condition requiring lifelong insulin, or a lifestyle-influenced condition that can be managed and even reversed, neither should be ignored.
Do not wait for symptoms to become serious before taking action. A simple blood test can tell you everything you need to know.
If you or someone in your family has been diagnosed with diabetes, or if you suspect your blood sugar may not be in a healthy range, I encourage you to get it checked. You can book a consultation with Dr. Dileep Verma at our Lucknow clinic. With over 20 years of experience in diabetes care, my goal is always the same: to help you understand your condition and take confident, informed steps toward better health.




