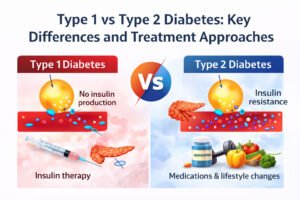
Most people think of diabetes as a sugar problem and fatty liver as a liver problem. But what if the two are more connected than you think? What if your liver is quietly sending you a warning, years before diabetes actually shows up?
This is not a coincidence. Fatty liver disease and Type 2 diabetes share the same root cause, and in many patients, one leads directly to the other. In this guide, we will explore the connection between fatty liver and diabetes, what you can do to catch it early, and how to stop it before it becomes diabetes. For expert diabetes and metabolic care in Lucknow, visit Dr. Dileep Verma’s clinic.
What is Fatty Liver Disease?
Fatty liver disease, also called hepatic steatosis, is a condition where excess fat accumulates in the liver cells. A small amount of fat in the liver is normal. But when fat makes up more than 5 to 10% of the liver’s total weight, it becomes a medical concern.
The liver is one of your body’s hardest working organs. It filters toxins, regulates blood sugar, produces proteins, and processes fats. When it gets overloaded with fat, it struggles to do all of these jobs properly, and the consequences go far beyond the liver itself.
Types of Fatty Liver
NAFLD (Non-Alcoholic Fatty Liver Disease):
This is the most common type and occurs in people who drink little to no alcohol. It is strongly linked to obesity, poor diet, insulin resistance, and sedentary lifestyle. This is the type most closely connected to diabetes risk.
AFLD (Alcoholic Fatty Liver Disease):
This is caused by excessive alcohol consumption, which disrupts how the liver processes and stores fat. While alcohol is the driver here, it can still contribute to metabolic complications including blood sugar dysregulation.
How Common is It?
Fatty liver disease affects approximately 25 to 30% of adults globally, making it the most common liver condition in the world. In India, studies suggest the prevalence is between 16 and 32%, and it is rising rapidly, especially in urban populations with sedentary lifestyles. According to the World Health Organization, the overlap between fatty liver and metabolic conditions like diabetes is a growing public health concern.
What Happens Inside a Fatty Liver?
Understanding what goes wrong inside a fatty liver helps explain why it is so closely linked to diabetes. It is not just about fat sitting there doing nothing. Fat in the liver actively disrupts some of the body’s most important processes.
The Role of the Liver in Blood Sugar Control
Your liver plays a central role in keeping your blood sugar stable throughout the day. Between meals, it releases stored glucose into the bloodstream to keep your energy levels up. After meals, it absorbs excess glucose and stores it as glycogen for later use.
Think of the liver as your body’s blood sugar regulator. It constantly monitors and adjusts glucose levels to keep things balanced. When the liver is healthy, this system works smoothly. When it is loaded with fat, that balance breaks down.
How Fat Buildup Disrupts Insulin
When fat accumulates in liver cells, it triggers inflammation and interferes with how the liver responds to insulin. Insulin is supposed to signal the liver to stop releasing glucose into the blood after a meal. But in a fatty liver, the liver ignores that signal. It keeps releasing glucose even when blood sugar is already high.
This is the beginning of insulin resistance, which is the foundation on which Type 2 diabetes is built.
The Fatty Liver and Diabetes Connection: How One Leads to the Other
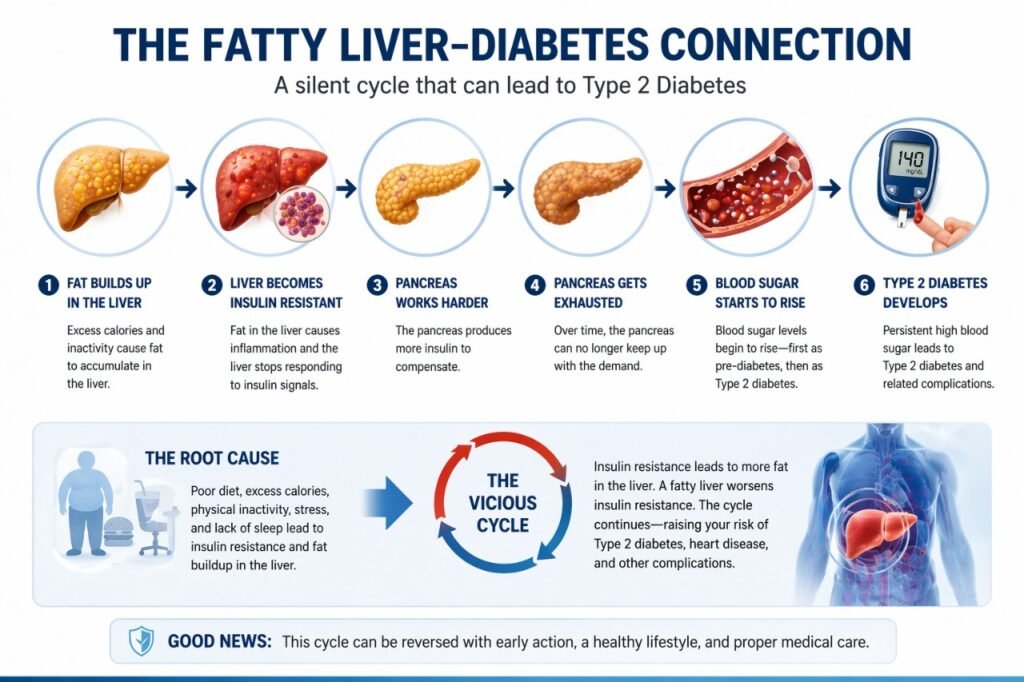
Fatty liver disease and Type 2 diabetes are so closely linked that researchers now describe them as two faces of the same underlying condition called metabolic dysfunction. Here is how the progression typically unfolds:
- Excess calories and inactivity cause fat to accumulate in the liver
- The fatty liver becomes resistant to insulin signals
- The pancreas works harder to produce more insulin to compensate
- Over time, the pancreas gets exhausted and can no longer keep up
- Blood sugar begins to rise, first as pre-diabetes, then as Type 2 diabetes
A Note from Dr. Verma
I see this pattern regularly in my clinic. A patient comes in for a routine check-up, we find a fatty liver on ultrasound, and their fasting blood sugar is already on the higher side. They had no symptoms. They felt completely fine. That is the danger with both conditions, they are silent until they are not silent anymore. If you have been told you have a fatty liver, please do not treat it as just a liver issue. Get your blood sugar and HbA1c checked at the same time.
Insulin Resistance: The Missing Link
Insulin resistance is the critical bridge between fatty liver and diabetes. When your liver, muscles, and fat cells stop responding normally to insulin, your pancreas compensates by producing more and more of it. For a while, this keeps blood sugar in a normal range. But insulin resistance and high insulin levels also promote more fat storage in the liver, creating a vicious cycle.
Left unaddressed, this cycle almost always ends in pre-diabetes and eventually Type 2 diabetes, along with a host of other complications including heart disease and kidney damage. According to the American Diabetes Association, insulin resistance driven by excess liver fat is one of the most common and preventable pathways to Type 2 diabetes.
Warning Signs You Should Not Ignore
One of the most challenging aspects of fatty liver disease is that it is almost entirely silent in its early stages. Most people have no idea they have it until it shows up on a routine scan or blood test. However, as the condition progresses, some signs may appear:
- Persistent fatigue and low energy that does not improve with rest
- A dull ache or discomfort in the upper right abdomen
- Unexplained weight gain, especially around the belly
- Bloating and a feeling of fullness even after small meals
- Elevated liver enzymes (ALT, AST) on blood tests
- Increased thirst and frequent urination, early signs of rising blood sugar
- Dark patches of skin on the neck or underarms (acanthosis nigricans), which is a sign of insulin resistance
A Note from Dr. Verma
What concerns me most is that many of my patients with fatty liver feel perfectly fine. They come in for something unrelated, maybe a routine check-up or a complaint about fatigue, and the ultrasound or blood test tells a different story. Do not wait for pain or discomfort to get tested. Fatty liver rarely hurts until it is already quite advanced.
Who is at Risk?
Fatty liver disease and its link to diabetes are more likely in people who have one or more of the following risk factors:
- Obesity or overweight, especially excess belly fat
- Type 2 diabetes or pre-diabetes already diagnosed
- High triglycerides or low HDL (good cholesterol)
- High blood pressure (hypertension)
- Sedentary lifestyle with very little physical activity
- Diet high in sugar, refined carbs, and processed foods
- Family history of liver disease or diabetes
- Polycystic ovarian syndrome (PCOS) in women
- Hypothyroidism or other hormonal conditions
If you have two or more of these risk factors, it is worth getting checked proactively. Early detection gives you the best chance to reverse the damage. Learn more about Dr. Dileep Verma’s diabetes and metabolic care services.
How is Fatty Liver Diagnosed?
Diagnosing fatty liver is straightforward when the right tests are done. Here are the most common approaches:
Liver Function Tests (LFTs)
A simple blood test that measures liver enzymes such as ALT (alanine aminotransferase) and AST (aspartate aminotransferase). Elevated levels suggest liver inflammation or damage and are often the first clue that something is wrong with the liver.
Ultrasound of the Abdomen
An abdominal ultrasound is the most commonly used imaging test for detecting fatty liver. It is non-invasive, painless, and can clearly show fat deposits in the liver. Most patients are first diagnosed through a routine ultrasound done for an unrelated complaint.
FibroScan and Liver Biopsy
A FibroScan (also called transient elastography) measures liver stiffness and can assess the degree of scarring (fibrosis) without a biopsy. In cases where the extent of liver damage is unclear, a liver biopsy may be recommended. This involves taking a small tissue sample for analysis and gives the most accurate picture of liver health.
Can Fatty Liver Be Reversed Before Diabetes Develops?
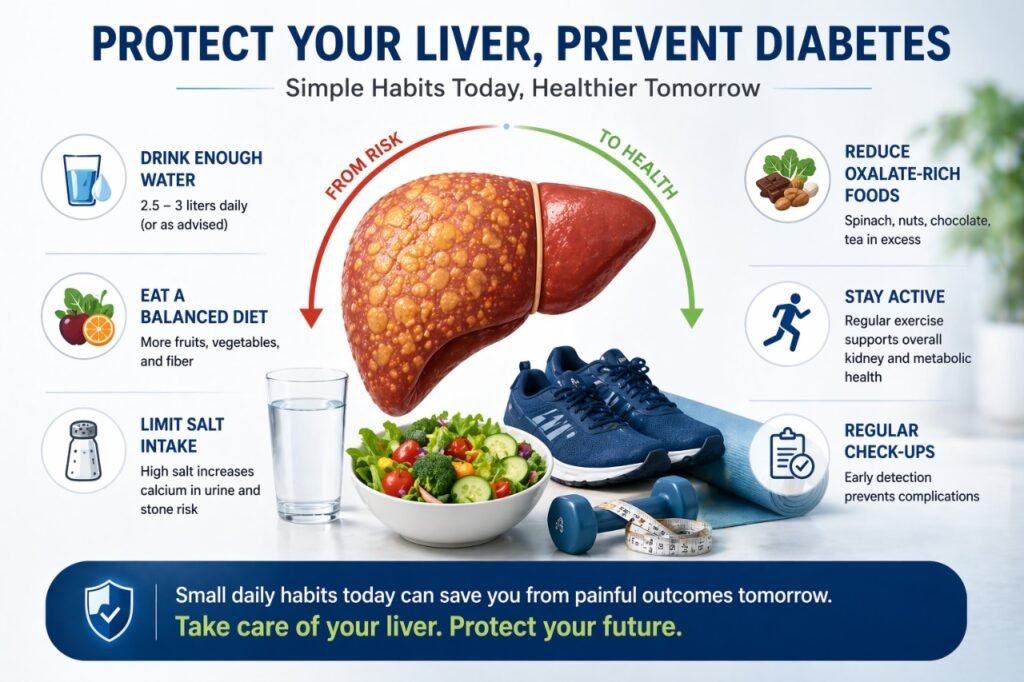
Yes, and this is the most hopeful part of this entire conversation. Unlike many chronic conditions, fatty liver disease caught early can be fully reversed through lifestyle changes alone, with no medication required in most cases. Even in more advanced stages, meaningful improvement is possible.
The key is acting before insulin resistance becomes full-blown diabetes. That window of opportunity is real, and it is worth every effort.
A Note from Dr. Verma
I always tell my patients who are diagnosed with fatty liver, this is your second chance. Your body is giving you a warning before things get serious. I have seen patients completely reverse their fatty liver within 6 to 12 months through diet changes and consistent exercise. The liver is one of the few organs in the body that can truly regenerate. Use that to your advantage.
Diet Changes
Reducing sugar, refined carbohydrates, and processed foods is the single most effective dietary change for reversing fatty liver. Replacing these with whole grains, vegetables, legumes, and healthy fats reduces the fat load on the liver and improves insulin sensitivity. A Mediterranean-style diet has shown particularly strong results in clinical studies.
Regular Exercise
Both aerobic exercise (walking, swimming, cycling) and strength training have been shown to reduce liver fat, even without significant weight loss. Aiming for at least 150 minutes of moderate activity per week is a good starting target. Even a 30-minute walk after dinner makes a meaningful difference over time.
Weight Loss
Losing just 5 to 10% of your body weight can significantly reduce liver fat and improve insulin sensitivity. For someone weighing 80 kg, that is just 4 to 8 kg. Gradual, sustainable weight loss through diet and exercise is far more effective than crash diets, which can actually worsen liver health.
Medication if Needed
In some cases, your doctor may recommend medications to manage associated conditions like high triglycerides, insulin resistance, or blood sugar. There is currently no single approved medication specifically for fatty liver, which is why lifestyle changes remain the cornerstone of treatment. Always discuss your options with a qualified diabetologist. Book a consultation with Dr. Dileep Verma here.
Foods That Harm vs Foods That Heal Your Liver
What you eat directly affects your liver. Here is a simple guide to help you make better choices every day:
| Foods That Harm Your Liver | Foods That Heal Your Liver |
| Sugary drinks: sodas, packaged juices | Leafy vegetables: palak, methi, broccoli |
| White bread, white rice, maida products | Whole grains: oats, brown rice, daliya |
| Fried and fast foods | Healthy fats: nuts, seeds, olive oil |
| Alcohol: even small amounts are harmful | Coffee: 2 cups a day may reduce liver fat |
| Packaged snacks high in trans fats | Fatty fish: omega-3 rich foods |
| Red and processed meats | Fruits low in sugar: berries, papaya, guava |
| High-fructose corn syrup products | Legumes: lentils, chickpeas, rajma |
Frequently Asked Questions
Can fatty liver directly cause diabetes?
Not directly, but it creates the conditions that lead to diabetes. Fatty liver causes insulin resistance, which forces the pancreas to overproduce insulin. Over time, the pancreas cannot keep up, and blood sugar begins to rise, first as pre-diabetes and then as Type 2 diabetes. The two conditions share the same metabolic root.
If I already have diabetes, can I still have fatty liver?
Yes, and it is very common. Studies show that 50 to 75% of people with Type 2 diabetes also have non-alcoholic fatty liver disease. Managing both conditions together is important, as uncontrolled fatty liver can make diabetes harder to manage and vice versa.
Is fatty liver painful?
Usually not in the early stages, which is why it often goes undetected. Some people may feel a dull discomfort in the upper right abdomen as the condition progresses, but many people have no symptoms at all until the liver is significantly damaged. This is why proactive testing matters.
How long does it take to reverse fatty liver?
With consistent diet changes and regular exercise, many patients begin to see measurable improvement in liver enzymes within 8 to 12 weeks. A full reversal, confirmed by ultrasound, typically takes 6 to 12 months depending on the severity. The earlier you start, the faster the results.
Do I need to avoid all fats if I have fatty liver?
No, and this is a common misconception. Healthy fats like those found in nuts, seeds, olive oil, and fatty fish are actually beneficial for liver health. It is the trans fats, saturated fats from processed foods, and excess sugar that drive fat accumulation in the liver. Focus on cutting sugar and refined carbs first.
Conclusion
Fatty liver is not just a liver problem. It is your body’s early warning system telling you that your metabolism is under stress, and that diabetes may not be far behind if nothing changes.
The encouraging truth is that this warning comes early enough to act on. Unlike many conditions that are difficult to reverse, fatty liver caught at the right time responds remarkably well to lifestyle changes. Your diet, your movement, and your awareness are your most powerful tools.
If you have been told you have a fatty liver, or if you have risk factors for it, do not wait for symptoms to appear. A simple ultrasound and blood test can give you the full picture. You can schedule a comprehensive metabolic evaluation with Dr. Dileep Verma at our Lucknow clinic. With over 20 years of experience in diabetes and metabolic care, the goal is always to help you understand your body and take informed steps before a warning becomes a diagnosis.